Indexed In
- The Global Impact Factor (GIF)
- CiteFactor
- Electronic Journals Library
- RefSeek
- Hamdard University
- EBSCO A-Z
- Virtual Library of Biology (vifabio)
- International committee of medical journals editors (ICMJE)
- Google Scholar
Useful Links
Share This Page
Journal Flyer

Open Access Journals
- Agri and Aquaculture
- Biochemistry
- Bioinformatics & Systems Biology
- Business & Management
- Chemistry
- Clinical Sciences
- Engineering
- Food & Nutrition
- General Science
- Genetics & Molecular Biology
- Immunology & Microbiology
- Medical Sciences
- Neuroscience & Psychology
- Nursing & Health Care
- Pharmaceutical Sciences
Review Article - (2021) Volume 20, Issue 10
Complications of Maxillofacial Distraction Osteogenesis: A New Classification System
Prajwalit Prakash Kende, Ashish Sunilkumar Sarda*, Neha Aggarwal, Harsh Desai, Jayant Landge and Varthangpuii
Abstract
Background: Widespread applications are possible with DO though it is a device dependant and technique sensitive procedure. With proper planning and execution, DO can become the gold standards for managing various maxillofacial disorders.
Aim: The aim of this literature review is to put forth a new classification system for the complications of distraction osteogenesis of facial skeleton.
Materials and methods: A detailed literature search was done on PUBMED, GOOGLE SCHOLAR and EMBASE from the year 1990 onwards. Any systematic review, randomized controlled trial, controlled clinical trial (CCT), retrospective/prospective study, literature of review classifying complications of distraction osteogenesis were included.
Results: Complications related to distraction osteogenesis classified by many authors including Paley, Samchukov, Mofid, Shetye, Norholt and Verlinden. Most of them were based on time, severity, tissues involved.
Conclusion: None of the given classification systems give a complete review on the complications and discuss the methods to prevent them. In this paper we intend to present a new comprehensive classification system of complications of DO which can be applied for avoiding complications in various phases of DO, decision making in their management and for the future studies related to maxillofacial DO.
Keywords
Distraction Osteogenesis, Complications, Classification, Maxillofacial, Surgery.
Introduction
Successful use of distraction osteogenesis (DO) on endochondral bones in 1950’s by Ilizarov [1] led to its application on the bones of the craniofacial region in the 1970’s. [2] Though initially used on the mandible, in recent years the maxilla, midface, orbits as well as cranial bones have been successfully distracted. DO is gaining widespread acceptance as a popular alternative to orthognathic surgery in the treatment of various craniofacial anomalies.
It is a technique sensitive procedure and is associated with a wide range of complications. A complication is an unexpected deviation from the treatment plan that, without appropriate correction, will lead to worsening of the existing, development of a new, or recurrence of the initial pathologic process. Maxillofacial DO is a device dependant and technique sensitive procedure, but with proper planning and execution, it can become the gold standard. The complications of DO were classified by several authors who discussed about their severity, ways of preventing them and need of intervention if needed. None of the complication system gives a complete review on the complications and discusses the methods to avoid them and/or manage them. The widespread application of DO in maxillofacial region in recent years has made it crucial to have a simple yet comprehensive complication system that will make the readers/ surgeons aware while planning or performing the procedure.
The purpose of this article is to present a new comprehensive classification of the complications of DO which can be applied for avoiding complications in various phases of DO, decision making in their management and for the future studies related to maxillofacial DO.
Material
Need for a New Classification
Presently, there are many classifications related to complications of DO. The main classifications which are used commonly are given by Paley, Samchukov, Mofid, Shetye, Norholt and Verlinden [3-8]. The advantages and disadvantages of the given classification systems are given in Table 1.
S.no |
Author |
Year |
Classification |
Points classification discuss about |
Points classification do not discuss about |
|---|---|---|---|---|---|
| 1 | Paley | 1990 | i. Problems. ii. Obstacles. iii. Complications. |
||
| 2 | M.Samchukov | 2001 | i. Mistakes (iatrogenic and patient related). ii. Complications (regenerate malformations, axial deviations, soft tissue overstretching, and infection). |
||
| 3 | Shetye | 2009 | i. Minor Incident. ii.Moderate Incident. iii. Major Incident. |
||
| 4 | Norholt | 2011 | i. No complications. Subclassification- a.Hardware related.b. Hard and soft tissue related. |
||
| 5 | Verlinden | 2015 | i.Type 1- spontaneously resolving complications. ii.Type 2- medically or technically manageable complication, without hospitalization. iii.Type 3- surgically manageable complication requiring local anaesthesia only, without hospitalization. iv. Type 4- technical complication, necessitating general anaesthesia for correction. v. Type 5- medically or surgically manageable complication with hospitalization or general anaesthesia. vi.Type 6-permanent sequelae, functionally and/or psychosocially disabling, and unachieved goal or unsatisfactory result. |
Table 1: Classification systems of complications of DO.
Paley in 1990 have given the first classification of complications of DO and was in use for almost a decade, it’s use have limited over a period of time due to very gross presentation of complications. M. Samchukov (2001) in his classification fails to discuss the severity of the complications and the urgency to manage them. The classification given by Mofid MM (2001) broadly divides the complications into five types based on his findings. There are no particular criteria given in his study to classify the complications. “Perioperative incident stratification” given by Shetye (2009) discusses complications based on their severity and the need of intervention. However, it fails to discuss them based on individual phases of distraction and urgency of management with same.
Norholt (2011) discussed about the relation of complications with the hardware and the hard and soft tissue, it again fails to lessen the disadvantages associated with the classification given by Shetye. Verlinden (2015) in his classification discussed the technical and surgical management of complications, the type of anaesthesia needed and their sequalae. Though this classification gives a brief idea about the management of complications classification, it fails to discuss their prevention.
It can be explained by the disadvantages of aforementioned classification systems that there is need of a classification system which discusses them based on individual phases of DO and time of occurrence of complications, with equal importance given to planning phase. Improper planning can lead to complications in other phases of DO, which if done correctly, may prevent many further complications. Also, the time of occurrence of the complications, can give the surgeon an idea about its urgency of management.
Our Proposed Classification
An ideal classification should be unambiguous, exhaustive, mutually exclusive, suitable, stable and flexible. At the same time, it should be simple, clear and universally adopted. Keeping above-mentioned things in mind, we have proposed a new classification system (Figure 1), named as “PK’s Classification of Complications of Maxillofacial Distraction Osteogenesis” based on individual phases of DO and their time of occurrence.
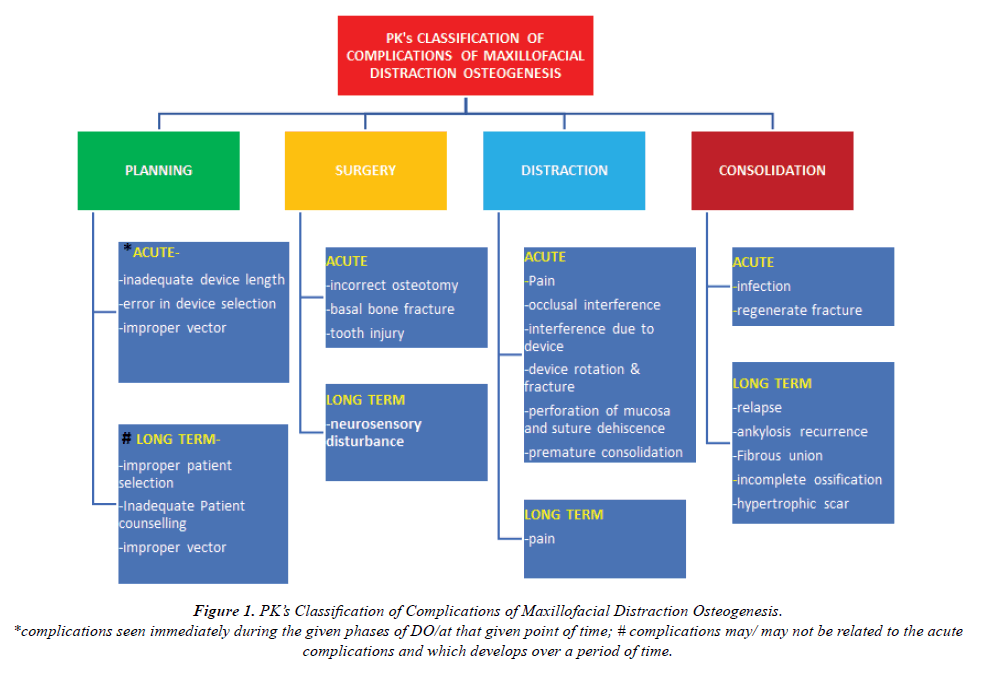
Figure 1: PK’s Classification of Complications of Maxillofacial Distraction Osteogenesis. *complications seen immediately during the given phases of DO/at that given point of time; # complications may/ may not be related to the acute complications and which develops over a period of time.
Complications Related to Planning Phase
Acute complications include inadequate device length, error in device selection and improper vector. Inadequate device length and error in device selection can cause insufficient correction (lengthening or failure in asymmetry correction) and failure during correction in single or multiple planes respectively. Long term complications include inadequate patient counselling, improper patient selection and improper vector. A non-compliant patient may activate the device more often or not at all leading to problems with regenerate formation. Also, if not counselled and managed properly May lead to broad range of consequences ranging from trifle ones like wound dehiscence, acute inflammation/ localised infection to significant ones like developing malocclusion and loosening or dismantling of the device. [9] Improper vector, though can be managed early, if left unmanaged may cause long term complications including malocclusion like laterognathism [presenting as cross bite(s)], anterior open bite, resorption of the condyle(s) and subsequently contributing towards development/ worsening of temporomandibular joint disorders (TMDs)] [10].
Complication Related to Surgery
Acute complications which may occur during surgery includes incorrect osteotomy, basal bone fracture and tooth injury. An incomplete osteotomy may ultimately lead to failure in obtaining the amount/ type of correction and distortion/ failure of the distractor. Excessive force delivered during completion of osteotomy can cause an unfavourable fracture of the basal bone which can add to the complexity of surgery. Presence of impacted tooth buds in the line of osteotomy or alternatively in the area of fixation of the device lies at a high risk of unintentional iatrogenic injury. Long term complications include neurosensory disturbance (NSD). NSD can be attributed to:
• Direct injury during osteotomy and distraction device application.
• Indirect damage such as focal nerve compression by progressive edema or device fixation elements.
Complications Related to Distraction Phase
Acute complications include pain, occlusal interference, and interference due to device, device rotation, device fracture and perforation of mucosa, suture dehiscence and premature consolidation. Device breakage and device rotation has been attributed to premature consolidation, improper activation, and external trauma to the device and unmanaged/ neglected occlusal discrepancies. There may be perforation of mucosa or dehiscence of suture due to improper vector of the device. Interference owing to the extension of the activated distraction device under the zygomatic arch in mandibular DO and interference of distraction arm with coronoid process in maxillary DO is a common problem. Premature consolidation is associated with inadequate rate of distraction and compressive forces on one side of the regenerate leading to early contact between osteotomized segments. Pain, can be an acute or a long-term complication and may be present due to high rate and rhythm of DO, due to discomfort with the intraoral activation rod of distractors, and long term due to pain associated with the regenerate.
Complication Related to Consolidation Phase
Acute complications include infection and regenerate fracture. Pin track infections are commonly associated with extraoral distractors and may be related to inadequate stability of the device and footplate screws during fixation. Regenerate fracture may occur due to:
• Inadequate duration of the consolidation period.
• Overaggressive functional rehabilitation during the remodelling period.
• Inadequate post-device removal immobilization when indicated.
• Excessive force applied to bone segments.
Long term complications include relapse, ankylosis recurrence, fibrous union, incomplete ossification and hypertrophic scar formation. Relapse can present clinically as quantitative or qualitative failures in the correction(s) achieved and subsequent development of occlusal discrepancies during consolidation. Temporomandibular joint (TMJ) sequelae have been noticed following mandibular distraction in older and syndromic patients who have pre-existing condylar pathologies, including degenerative arthrosis of the articulating surfaces, increased woven bone formation, irregularities of the articulating cartilage, and ultimately TMJ ankylosis. Incomplete ossification may occur in in patients of older age, habitual smokers, compromised oral hygiene conditions, with irradiated jaw(s), with higher rate of distraction and removal of distractor before the complete mineralization of the newly formed bone.
Results and Discussion
Out of several complications given in literature till date the common shortcomings were that the complications were not discussed based on:
• The phases of distraction, most importantly the planning phase
• Time of occurrence.
With our new classification system, we have made an effort to circumvent the common disadvantages of the already available classification systems.
Paley has classified complications as problems, obstacles and complications based on need of intervention. However, this classification poorly defines the complications, based on its phase and time of occurrence. Also, it becomes cumbersome to the reader or operator to have an idea about same.
M. Samchukov has discussed mistakes along with the complications, defining mistakes as a different entity. He defined it as “an inattentive action that results in a deviation of course of the treatment, thereby leading to the development of a complication”. Mistakes may either be iatrogenic or patient related. He divided complications into regenerate malformation, axial deviation, soft tissue overstretching and infection. This classification gives a brief idea about the complication and mistakes; however, it fails to discuss them based on phases and time of occurrence, their severity and urgency of management.
Mofid MM has broadly divided complications in five types based on his retrospective study involving 3,278 cases. This classification fails to discuss the complications based on
• Individual phases of DO
• Its severity
• Urgency of their management.
Use of this classification is very limited in the field of maxillofacial DO.
“Perioperative Incident Stratification” given by Shetye discusses the complications based on their severity as minor, moderate and major incident. This classification also gives an idea about the need for conservative or surgical management with same. However, it fails to discuss them based on individual phases of distraction, their time of occurrence and urgency of their management.
Norholt have modified the classification given by Shetye by further dividing each complication into:
• Hardware related and,
• Hard and soft tissue related.
He also changed the word ‘incident’ given in later classification to ‘complications’. However, it fails to lessen the disadvantages associated with later classification.
Verlinden in his “Distraction Osteogenesis Classification Index” have divided the complications in six types based on their management, where type 1 complications are spontaneously resolving while type 6 complications are the permanent sequalae, functionally and/or psychologically disabling with unsatisfactory results. This complication discusses the technical and surgical management of complications, the type of anesthesia needed and their sequalae. However, this classification doesn’t discuss the complications based on individual phases of DO, time of their occurrence and urgency of management.
Based on above discussion, we can clearly figure out the cons of the classifications given till date. Most of the classifications fail to discuss the complications based on:
• Individual phases of DO.
• Time of their occurrence, and
• Urgency of their management.
To circumvent the disadvantages of the given classification systems, our classification discusses the complications based on the individual phase and the time of occurrence of DO. Based on individual phase, complications were divided into those occurring during planning, surgery, distraction and consolidation. We have given special consideration to planning phase as no other classification system discusses its importance in the prevention and management of further developing complications. Complications in planning phase are imparted to improper patient selection and counselling, errors in device selection, inadequate device length and improper vector. Keeping these complications in mind, planning the procedure systematically, can improve the outcome of surgery.
We further divided each phase into acute and long term based on time of occurrence. Acute complications seen immediately during the given phases of DO/at that given point of time; Long term complications may/ may not be related to the acute complications and which develops over a period of time. Dividing complications based on time, will give an idea about their occurrence and urgency of management.
Conclusion
The disadvantages of the classification systems given in the literature till now signify the need for a systematic and flexible classification system, which will be universally acceptable and be easily adaptable. We hope that this new classification system can be applied to avoid complications in different phases of maxillofacial DO, decision making in their management and for the future studies by the researchers and surgeons worldwide for various purposes.
Compliance with Ethical Standards
Funding
No funding received.
Conflict of Interest
No conflict of interest declared by all the authors.
Ethical Approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed Consent
This article does not contain any studies with human participants or animals performed by any of the authors
REFERENCES
- Ilizarov GA. The tension-stress effect on the genesis and growth of tissues. Part I. The influence of stability of fixation and soft-tissue preservation. Clinical Orthopaedics and Related Research. 1989; 238: 249-281.
- Snyder CC, Levine GA, Swasson HM, Browne JREZ. Mandibular lengthening by gradual distraction: preliminary report. Plastic and Reconstructive Surgery. 1973; 51: 506-508.
- Alexander C, Mikhail S. Potential mistakes and complications. In: samchukov ml, cope jb, cherkashin am (eds) Craniofacial distraction osteogenesis. Oral Surgery. 2001: 581-594.
- Paley D. The correction of complex foot deformities using Ilizarov's distraction osteotomies. Clinical Orthopaedics and Related Research. 1993; 293: 97-111.
- Mofid MM, Manson PN, Robertson BC, Tufaro AP, Elias JJ. Craniofacial distraction osteogenesis: A review of 3278 cases. Plastic and Reconstructive Surgery. 2001; 5: 1103-1114.
- Shetye PR, Warren SM, Brown D, Garfinkle JS, Grayson BH. Documentation of the incidents associated with mandibular distraction: Introduction of a new stratification system. Plastic and Reconstructive Surgery. 2009; 123: 627-634.
- Nørholt SE, Jensen J, Schou S, Pedersen T K. Complications after mandibular distraction osteogenesis: A retrospective study of 131 patients. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology. 2011; 111: 420-427.
- Verlinden CRA, van de Vijfeijken SECM, Tuinzing DB, Becking AG. Complications of mandibular distraction osteogenesis for acquired deformities: A systematic review of the literature. International Journal of Oral and Maxillofacial Surgery. 2015; 44: 956-964.
- Troulis MJ, Kaban LB. Complications of mandibular distraction osteogenesis. Oral and Maxillofacial Surgery Clinics. 2003; 15: 251-264.
- Master DL, Hanson PR, Gosain AK. Complications of mandibular distraction osteogenesis. Journal of Craniofacial Surgery. 2010; 21: 1565-1570.
