Indexed In
- RefSeek
- Hamdard University
- EBSCO A-Z
- Publons
- Euro Pub
- Google Scholar
- Quality Open Access Market
Useful Links
Share This Page
Journal Flyer

Open Access Journals
- Agri and Aquaculture
- Biochemistry
- Bioinformatics & Systems Biology
- Business & Management
- Chemistry
- Clinical Sciences
- Engineering
- Food & Nutrition
- General Science
- Genetics & Molecular Biology
- Immunology & Microbiology
- Medical Sciences
- Neuroscience & Psychology
- Nursing & Health Care
- Pharmaceutical Sciences
Research Article - (2026) Volume 12, Issue 1
Incidence and Predictors of Moderate to Severe Postoperative Pain after Cesarean Section among Parturient Receiving Spinal Anesthesia at the Selected Southern Ethiopian Governmental Hospital 2023: A Multicenter Prospective Single-Armed Cohort Study
Dejene Moreda1*, Yonas Sagni2, Hunde Amsalu1 and Simeneh Molla32Department of Midwifery, College of Medicine and Health Sciences, Wachemo University, Hossana, Ethiopia
3Department of Anesthesia, College of Medicine and Health Sciences, Dilla University, Dilla, Ethiopia
Received: 09-Sep-2024, Manuscript No. JPMME-24-26877; Editor assigned: 05-Sep-2024, Pre QC No. JPMME-24-26877 (PQ); Reviewed: 19-Sep-2024, QC No. JPMME-24-26877; Revised: 04-Feb-2026, Manuscript No. JPMME-24-26877 (R); Published: 11-Feb-2026, DOI: 10.35248/2684-1320.26.12.366
Abstract
Background: Inadequate treatment of postoperative pain predisposes patients to delayed recovery, affects the interaction between mothers and babies, results in longer hospital stays, and increases the incidence of chronic pain. In limited resource areas, postoperative pain management is challenging because of the inadequate administration of pain relief drugs and the high patient-to-nurse ratio, which limits the assessment of pain. Objective: To assess the incidence and predictors of moderate to severe postoperative pain after cesarean section among parturients receiving spinal anesthesia at selected Southern Governmental Hospitals from January 1 to May 30, 2023.
Methods: A multicenter prospective cohort study was conducted at selected hospitals after ethical approval was obtained from the institutional review board. A numeric rating scale was used to assess pain severity. Binary logistic regression was used to identify independent risk factors for postoperative pain. A p value of 0.05 was considered the cutoff point to test for statistical significance in multivariate logistic regression analysis.
Results: In our study, the incidence of moderate to severe postoperative pain after cesarean section was 68.29% within the first 24 hours. On the basis of the multivariable analysis, preoperative anxiety (AOR: 2.849, 95% CI: 1.276, 6.359), previous cesarean section (AOR: 3.571, 95% CI: 1.536, 8.300) and transverse incision (AOR: 6.965, 95% CI: 2.469, 19.652) were significantly associated with moderate to severe postoperative pain after cesarean section. Abdominal field blocks decreased the incidence of postoperative pain (AOR: 0.035, 95% CI: 0.009, 0.139).
Conclusion: In this study, many parturients experienced moderate to severe postcaesarean pain in the first 24 hours. Preoperative anxiety, a history of previous cesarean section, and a transverse incision were predictors of moderate to severe postcaesarean pain. Postoperative pain should be assessed, and interventions should be given on the basis of the severity of pain according to pain scale assessment.
Keywords
Post caesarean section pain; Pain; Cesarean section; Postoperative pain
Introduction
A Cesarean Section (CS) is one type of delivery in which a surgical incision is made into the mother’s abdomen and uterus [1]. It is one of the most commonly performed procedures in obstetrics practice for saving the lives of mothers and their newborns who are receiving general or neuraxial anesthesia [2]. The World Health Organization (WHO) recommends that the regional CS rate should not exceed 10-15%; however, the percentage of cesarean sections is significantly elevated globally [3,4].
Pain is defined as a sensory and emotional experience associated with actual or potential tissue damage or is described in terms of such damage [5]. It is a main issue in cesarean section [6]. Poor management of pain is common and can have serious consequences. Untreated postoperative pain may result in clinical and psychological changes that increase morbidity and mortality while also decreasing quality of life [7].
Approximately 20% of parturients develop moderate to severe postoperative pain following cesarean section. These mothers may complain of severe pain for months after cesarean section [8]. These parturients may never stop receiving the opioids they are prescribed [9].
Women who experience moderate to severe postoperative pain following cesarean section can delay recovery and return to daily activities, affect maternal psychological well-being, increase hospital stays, chronic postoperative pain, complicate breastfeeding, and increase medical costs, all of which increase medical costs and are emerging as public health concerns. This is a growing public health concern for us.
Ineffective postoperative pain management following a cesarean section hurts mobilization, increased morbidity, impaired physical function and quality of life, prolonged opioid use during and after hospitalization, increased costs of care, and the absence of an early motherâ??infant bond, all of which harm the development of the baby.
After a cesarean section, pain with movement remains unfocused while being more severe than pain at rest and possibly requiring the administration of multiple medications. There is an increased risk of thromboembolic complications, persistent pain, and postpartum depression, which affect the fetal population of parturients; therefore, early mobilization is important. Early recovery is especially important for a pregnant woman who is able to have her baby after an operative procedure.
Pain after surgery is often very intense, especially in the first six hours after the procedure. The use of safe and efficient analgesic combinations to provide adequate pain relief to women after cesarean section is a common concern. There are various possibilities, and the selection of a pain management technique is influenced by the availability of drugs, institutional protocols, personal preferences, the availability of resources, and financial concerns.
Although new analgesics and delivery methods have been developed, many patients still experience moderate to severe postoperative pain following cesarean sections. The lack of specialized pain management services, as well as the lack of information and negative attitudes toward pain among patients and medical staff, have all been cited in studies as the root causes of this issue.
Owing to patients' expectations of postoperative pain and the low nurse-to-patient ratio, which restricts the assessment of pain and the administration of effective pain relief medications, postoperative pain management can be particularly difficult in low-income nations.
A study conducted in Ethiopia on the prevalence of postoperative pain among surgical patients revealed that postsurgical pain is still severe and that there is inadequate pain management. Designing factor-specific therapies to alleviate patient suffering may be made possible by identifying perioperative factors related to the incidence of moderate to severe postoperative pain.
Very little is known about the incidence and predictors of postoperative pain in developing countries. In particular, no studies have been conducted regarding the incidence and predictors of postoperative pain after cesarean delivery in patients undergoing spinal anesthesia in Ethiopia. A few studies have reported the overall incidence of postoperative pain among surgical patients undergoing different procedures and compared different methods of analgesia. Therefore, in resource-limited areas, it is essential to know the incidence and predictors of postoperative pain to plan appropriate interventions and adequate utilization of basic analgesic modalities.
Materials and Methods
Study design and area
A multicenter prospective single-armed cohort study was conducted from January 2023-May 2023 at selected Southern Ethiopia governmental teaching hospitals, Dilla University Referral Hospital and Hawassa University Comprehensive Specialized Hospital. Dilla University Referral Hospital is located in the Gedeo Zone, Southern Nation Nationality and People’s Regional State (SNNPRS), Ethiopia. Hawassa University Comprehensive Specialized Hospital is located in Hawassa city in the Sidama Region, Ethiopia.
Population
The study population included all parturients who underwent cesarean section under spinal anesthesia at Dilla University Referral Hospital and Hawassa University Comprehensive Specialized Hospital from January 1 to May 30, 2023. Parturients who had preexisting cognitive dysfunction and failed spinal anesthesia were excluded from this study.
Sample size and sampling technique
Sample size calculation: The sample size estimate based on a previous study of the incidence of postcaesarean pain during the first 24 hours was 85.5%, which was taken from a study conducted at the University of Gondar Comprehensive Specialized Hospital (UOGCSH), Ethiopia.
A single proportion formula with a 95% level of significance, a 5% margin of error, and a 10% margin of error for incomplete or contingency data was used as the parameter. When a 10% nonresponse rate was added, the total sample size was 20.
Sampling technique: A situational analysis was performed on the basis of the recorded logbooks of cesarean sections performed for the last three months in both hospitals. On average, 247 C/S patients at DURH and 436 at HUCSH underwent cesarean section every three months. Finally, the sample size was allocated proportionally to both hospitals on the basis of their average three-month reporting.
Therefore, during the study period, a total of 683 patients underwent a cesarean section. Since the calculated sample size was 209, the value of 683 divided by 209 was 3.3. A systematic sampling technique was used.
Methods of data collection
Through the use of a pretested structured questionnaire, data were collected. The questionnaire was prepared in both the English language and the Amharic language. A pretested questionnaire was given to 5% of the parturients at Dilla University referral hospital. After the patient arrived at the postanaesthesia care unit, the presence of postoperative pain was assessed at the 2nd, 6th, 12th, and 24th postoperative hours via the NRS.
Preoperative, intraoperative, and postoperative data were collected by 2 trained BSc anesthetists and 2 BSc midwives. The data collectors provided informed consent, interviewed the patients, reviewed the charts, and documented pain severity via the NRS-11.
Study variables
The dependent variable was the incidence of postoperative pain (no to mild pain and moderate to severe postoperative pain). The independent variables were socio-demographics (age, BMI, religion, educational status, marital status, employment status), preoperative factors (ASA classification, current smoker, preoperative anxiety, analgesics given, previous scars, parity, blood type, coexisting disease), intraoperative factors (analgesia given, incision type and length, duration of surgery, emergency or elective cesarean section) and postoperative factors (types of analgesia given).
Operational definition
A Numerical Rating Scale with 11 points (NRS-11) is a valid and reliable pain assessment tool in which the numbers are assigned from 0–10 to represent the severity of pain: 0=no pain, 1– 3=mild pain, 4–6=moderate pain, and 7–10=severe pain. In this study, the NRS-11 was preferred because of its simplicity of understanding by parturients. A tolerable pain threshold is defined as a treatment threshold of a pain score with a cutoff point of NRS-11 ≥ 4, which is considered to identify patients with moderate to severe pain.
Moderate to severe postoperative pain: When a patient experiences moderate to severe postoperative pain in the first 24 postoperative hours with a cutoff point of NRS ≥ 4, this cutoff point was identified as the tolerable pain threshold.
Preoperative anxiety: S-STAI scores indicate anxiety and no anxiety.
There is anxiety: Patients who score on the S-STAI>44.
Low/no anxiety: Patients who score on the S-STAI ≤ 44.
The six-item short-form of the STAI produces scores similar to those achieved via the full 20-item STAI. It has standard reliability and produces scores that are similar to those produced with the full-form across subject groups, indicating normal and elevated levels of anxiety. A brief questionnaire decreases the time taken to complete the questionnaire and the time taken to score the results.
Data quality assurance
The data collectors received brief orientations on the assessment tools as well as training on the goals and applicability of the study to ensure the quality of the data. Data were gathered via a structured and pretested questionnaire after the data collectors had received training. Each questionnaire was reviewed by the investigator throughout the data collection process to ensure that it was complete and appropriate.
Data analysis procedure
The data were coded and then entered, cleaned, and edited via Statistical Package for Social Sciences (SPSS) software version. Using SPSS, basic descriptive statistics such as frequency and cumulative frequency were calculated for sociodemographic variables and the incidence of postoperative pain, respectively. A numeric rating scale was used for the assessment of pain severity. Binary logistic regression was used to identify independent risk factors for postoperative pain. The data were tested for a normal distribution by using the Shapiro-Wilk test and a histogram for continuous variables. The median and interquartile range were used for nonnormally distributed variables. The Hosmer– Lemeshow test was used for goodness-of-fit. Multicollinearity was checked by the tolerance value and variance inflation factor (for each independent variable). The associations between independent factors and the outcome variable were determined at the 95% CI with bivariate and multivariate binary logistic regression. The strength of the statistical association was measured by an adjusted odds ratio and a 95% confidence interval. Variables with a p value less than 0.25 in the bivariate binary logistic analysis were included in the multivariate binary logistic regression analysis, and a p value of 0.05 was considered the cutoff point to test for statistical significance. In multivariate binary logistic regression, variables with a p value of 0.05 were statistically significant. The results are presented in text, tables, charts, and graphs.
Results
Among the 209 study participants who were recruited for this study, four participants were excluded because of failed spinal anesthesia. A total of 205 participants were included in the analysis. Data were gathered from 130 parturients at HUCSH and 75 parturients at DURH.
Socio-demographic characteristics
The median and Interquartile Range (IQR) of parturients’ ages were 27 and 25–30, respectively. The median and Interquartile
Range (IQR) of the parturients’ body mass index were 24 and 22–27.25, respectively. The majority of the parturients, 181 (91.2%), were between the ages of 18 and 34 years, and the body mass index of 106 (51.7%) parturients was in the range of 18.5– 24.9 kg/m2. The majority of the parturients were protestant (91 (44.4%)) and married (197 (96.1%)). The majority of the parturients, 66 (32.2%), were merchants, and 63 (30.7%) of them had only a primary education (Table 1).
| Variables | Frequency (n) | Percentage (%) | |
| Age | 18-34 | 187 | 91.2 |
| 35 | 18 | 8.8 | |
| BMI | <18.5 | 2 | 1 |
| 18.5
≥ 24.9 |
106 | 51.7 | |
| 25-29.9 | 77 | 37.6 | |
| 30-39.9 | 20 | 9.8 | |
| Marital status | Married | 197 | 96.1 |
| Unmarried | 3 | 1.5 | |
| Divorced | 5 | 2.4 | |
| Religion | Orthodox | 64 | 31.2 |
| Muslim | 50 | 24.4 | |
| Protestant | 91 | 44.4 | |
| Educational | No formal education | 27 | 13.2 |
| Primary education | 63 | 30.7 | |
| Secondary education | 56 | 27.3 | |
| College and university | 59 | 28.8 | |
| Occupational | Farmer | 17 | 8.3 |
| Merchant | 66 | 32.2 | |
| Employed | 51 | 24.9 | |
| Student | 8 | 3.9 | |
| Unemployed | 53 | 25.9 | |
| Others | 10 | 4.9 | |
Table 1: Sociodemographic characteristics of the parturients who delivered via cesarean section at both hospitals in Southern Ethiopia; 2023 (N=205).
Perioperative factors
Among 205 parturients, 177 (86.3%) were ASA II. The majority of the parturients (113/55.1%) had no previous cesarean section scars. The majority of the parturients, 145 (70.7%), were multiparous, and 83 (40.5%) of them had blood type O. Threefourths of the parturients, 153 (74.6%), were term pregnant. The majority, 167 (81.5%) of the parturients who underwent C/S under spinal anesthesia, came to the operating room for an emergency C/S, and 174 (84.9%) of the parturients underwent a transverse incision. The duration of surgery for the 174 parturients who underwent C/S was less than 60 minutes. A single analgesic approach was used to address postoperative pain in the majority of our research participants. This was a factor in the increase in postoperative pain complaints following cesarean delivery. In hospitals, abdominal field blocks, such as TAP blocks and IL/IH nerve blocks, are the most widely used regional analgesic alternatives for postoperative pain management following CS. However, these abdominal field blocks were performed in only approximately 25 (12.2%) parturients, while the remaining 180 (87.8%) parturients had not received abdominal field blocks (Table 2).
| Variables | Frequency (n) | Percentage (%) | |
| ASA | ASA II | 177 | 86.3 |
| ASA III | 28 | 13.7 | |
| Previous c/s scar | Yes | 92 | 44.9 |
| No | 113 | 55.1 | |
| Preoperative anxiety | Yes | 79 | 38.5 |
| No | 126 | 61.5 | |
| Parity | Nulliparous | 60 | 29.3 |
| Multiparous | 145 | 70.7 | |
| Blood type | Type A | 38 | 18.5 |
| Type B | 68 | 33.2 | |
| Type O | 83 | 40.5 | |
| Type AB | 16 | 7.8 | |
| Gestational age | <37 weeks | 15 | 7.3 |
| 37-42 weeks | 153 | 74.6 | |
| >42 weeks | 37 | 18 | |
| Coexisting diseases | Yes | 21 | 10.2 |
| No | 184 | 89.8 | |
| Urgency of c/s | Emergency | 167 | 81.5 |
| Elective | 38 | 18.5 | |
| Types of incision | Transverse | 174 | 84.9 |
| Vertical | 31 | 15.1 | |
| Duration of surgery | ≥ 60 minutes | 31 | 15.1 |
| <60 minutes | 174 | 84.9 | |
| Abdominal field blocks | Yes | 25 | 12.2 |
| No | 180 | 87.8 | |
Table 2: Distributions of perioperative factors in parturients who underwent cesarean section under spinal anesthesia at both hospitals.
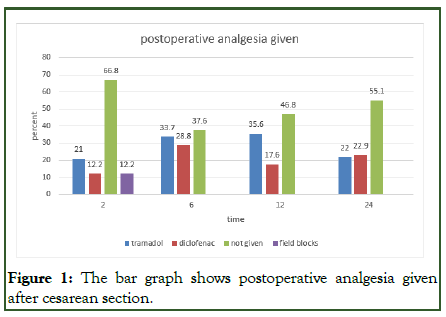
According to postoperative pain management in this study, approximately 137 (66.8%) of the parturients received no analgesics in the second hour. Of the total 68 (43.2%) parturients who used analgesics at that time, 43 (21%) had used tramadol. In the sixth hour, more parturients were given analgesics. The main systemic analgesics used to relieve pain were diclofenac and tramadol, which were given to approximately 128 (62.5%) parturients. At the 12th hour, approximately 96 (46.8%) of the parturients were without analgesics. Approximately 113 (55.1%) parturients had not received any analgesics at the 24th hour (Figure 1).
Figure 1: The bar graph shows postoperative analgesia given after cesarean section.
The severity of postoperative pain according to the NRS score
The proportion of parturients reporting moderate to severe postoperative pain on a numerical rating scale was 71 (34.6%) at 2 hours, 125 (61%) at 6 hours, 108 (52.7%) at 12 hours, and 84 (41%) at 24 hours following cesarean birth. The median and interquartile range for postoperative pain were 2 hours (3, 0–4), 6 hours (5, 2–7), 12 hours (4, 2–7), and 24 hours (2, 1–4) after cesarean section surgery, respectively. The highest median for postoperative pain at 6 hours was 5, which was greater than that at the other time points.
Incidence of postoperative pain
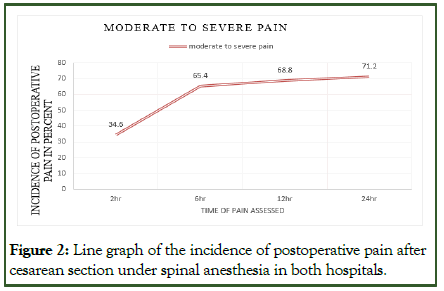
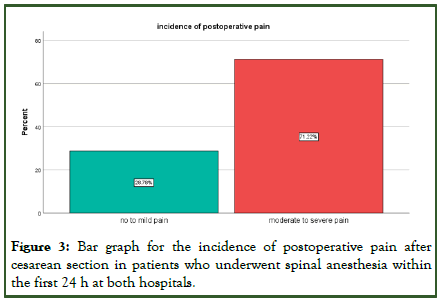
In this study, 71 (34.6%) of the participants experienced moderate to severe pain during the first 2 hours after a cesarean section, and 134 (65.4%) patients reported experiencing moderate to severe pain during the first 6 hours after a cesarean section. The incidence of postoperative pain during the first 12 hours was 141 (68.8%) participants who reported moderate to severe pain. Within the first 24 hours after a cesarean section, 146 parturients (71.2%) experienced moderate to severe pain (Figures 2 and 3).
Figure 2: Line graph of the incidence of postoperative pain after cesarean section under spinal anesthesia in both hospitals.
Figure 3: Bar graph for the incidence of postoperative pain after cesarean section in patients who underwent spinal anesthesia within the first 24 h at both hospitals.
Predictors of moderate to severe postoperative pain after cesarean section
Multivariate logistic regression analysis revealed that a history of preoperative anxiety, previous c/s scar, transverse incisions, and abdominal field blocks were significantly associated with moderate to severe postoperative pain after cesarean section.
The parturients who experienced preoperative anxiety were 2.849 times (AOR: 2.849, 95% CI: 1.276, 6.359) more likely to develop moderate to severe postoperative pain than those who were not anxious. Parturients who had a history of previous C/S scars were 3.571 times (AOR: 3.571, 95% CI: 1.536, 8.300) more likely to develop moderate to severe postoperative pain than those who had no history of previous C/S scars. Our results also revealed that parturients who had undergone a transverse incision were 6.965 times (AOR: 6.965, 95% CI: 2.469, 19.652) more likely to develop moderate to severe postoperative pain than those who had undergone a vertical skin incision. Compared with those who did not receive abdominal field blocks, parturients who received postoperative abdominal field blocks 0.035 times (AOR: 0.035, 95% CI: 0.009, 0.139) less likely to experience moderate to severe pain (Table 3).
| Variables | No to mild pain | Moderate to severe pain | Crude OR (95% CI) | Adjusted OR (95% CI) | P-values | |
| Educational | No formal education | 7 (25.9%) | 20 (74.1%) | 1 | 1 | 0.117 |
| Primary education | 17 (27%) | 46 (73%) | 0.947 (0.34, 2.63) | 0.486 (0.12, 1.95) | ||
| Secondary education | 16 (28.6%) | 40 (71.4%) | 0.875 (0.31, 2.47) | 0.443 (0.10, 1.79) | ||
| College and above | 25 (42.4%) | 34 (57.6%) | 0.476 (0.17, 1.29) | 0.318 (0.07, 1.33) | ||
| Occupational | Farmer | 4 (23.5%) | 13 (76.5%) | 1 | 1 | 0.09 |
| Merchant | 23 (34.8%) | 43 (65.2%) | 0.575 (0.16, 1.96) | 0.205 (0.03, 1.07) | ||
| Employed | 16 (31.4%) | 35 (68.6%) | 0.673 (0.19, 2.39) | 0.476 (0.08, 2.58) | ||
| Student | 5 (62.5%) | 3 (37.5%) | 0.185 (0.03, 1.13) | 0.121 (0.01, 1.39) | ||
| Unemployed | 14 (26.4%) | 39 (73.6%) | 0.857 (0.23, 3.07) | 0.646 (0.12, 3.38) | ||
| Others | 3 (30%) | 0.718 (0.12, 4.15) | 0.292 (0.02, 3.01) | |||
| ASA | ASA II | 58 (32.8%) | 119 (67.2%) | 1 | 1 | 0.285 |
| ASA III | 7 (25%) | 21 (75%) | 2.108 (0.68, 6.53) | 2.203 (0.51, 9.36) | ||
| BMI | <30 kg/m2 | 61 (33.2%) | 123 (66.8) | 1 | 1 | 0.146 |
| ≥ 30 kg/m2 | 4 (19%) | 17 (81%) | 2.108 (0.68, 6.53) | 2.729 (0.70, 10.57) | ||
| Preoperative anxiety | No | 49 (38.9%) | 77 (61.1%) | 1 | 1 | 0.011 |
| Yes | 16 (20.3%) | 63 (79.7%) | 2.579 (1.34, 4.96) | 2.849 (1.27, 6.35) | ||
| Previous c/s scar | No | 41 (36.3%) | 72 (63.7%) | 1 | 1 | 0.003 |
| Yes | 24 (26.1%) | 68 (73.9%) | 1.613 (0.88, 2.94) | 3.571 (1.53, 8.30) | ||
| Types of incision | Vertical | 14 (45.2%) | 17 (54.8%) | 1 | 1 | |
| Transverse | 51 (29.3%) | 123 (70.7%) | 1.986 (0.91, 4.32) | 6.965 (2.46, 19.65) | 0 | |
| Abdominal field blocks | No | 44(24.4%) | 136(75.6%) | 1 | 1 | |
| Yes | 21(84%) | 4(16%) | 0.062 (0.02, 0.18) | 0.035 (0.009, 0.13) | 0 | |
| Gestational age | Term | 50 (32.7%) | 103 (67.3%) | 1 | 1 | |
| Preterm | 7 (46.7%) | 8 (53.3%) | 0.555 (0.19, 1.61) | 0.594 (0.15, 2.21) | ||
| Post term | 8 (21.6%) | 29 (78.4%) | 1.760 (0.75, 4.12) | 1.705 (0.61, 4.72) | 0.305 | |
| Blood types | Type A | 8 (21.1%) | 30 (78.9%) | 1 | 1 | |
| Type B | 25 (36.8%) | 43 (63.2%) | 0.459 (0.18, 1.15) | 0.494 (0.15, 1.56) | 0.23 | |
| Type O | 25 (30.1%) | 58 (69.9%) | 0.619 (0.24,1.53) | 0.364 (0.11, 1.17) | ||
| Type AB | 7 (43.8%) | 9 (56.3%) | 0.343 (0.09, 1.20) | 0.482 (0.10, 2.30) | ||
Table 3: Bivariate and multivariate binary logistic regression showing factors associated with postoperative pain after cesarean section at both hospitals from March to May 2023.
Discussion
On the basis of the findings of our study, at four time points, the incidence of moderate to severe postoperative pain was 71 (34.6%) within 2 hours, 134 (65.4%) after 6 hours, 141 (68.8%) after 12 hours, and 146 (71.2%) after 24 hours of cesarean section delivery. We found that preoperative anxiety, previous cesarean section, and transverse incisions were significant predictors of moderate to severe pain after cesarean section.
We found that the incidence of moderate to severe pain within 24 hours after a cesarean section was 71.2%. A study conducted in northwest Ethiopia revealed that the incidence of moderate to severe post-Cesarean section pain was 85.5% (95% CI: 81.4%, 89.0%) within the first 24 hours. In the above study, the incidence of moderate to severe postoperative pain was greater than that reported in our study. The possible explanation for this variation is that the above study had a larger sample size than our study did, and their study population included both spinal and general anesthesia. The reason for the lower incidence of pain in our study might be the relatively small sample size and the fact that the study population included only those who underwent spinal anesthesia.
A prospective longitudinal study performed in Brazil revealed that the incidence of moderate to severe postoperative pain after cesarean section was 78.4% (CI: 95%: 75.9%–80.8%). In the above study, the incidence of moderate to severe postoperative pain after cesarean section was slightly greater than that reported in our study. The possible explanation for this variation is that they used a larger sample size than our results did. The possible reason for the lower incidence of pain in our study might be the relatively small sample size.
A prospective cohort study conducted in the United States revealed that the prevalence of severe postoperative pain after cesarean section was 10.9% within 36 hours. On the basis of the above findings, the incidence of moderate to severe postoperative pain was much lower than previously reported. The possible explanation for this variation is that better pain management and pain assessment practices may be the cause of this difference when we compare our results to theirs.
According to a prospective descriptive survey conducted in Uganda, the incidence of moderate to severe pain following cesarean surgery at three time intervals was 23%, 39%, and 29%, respectively, at zero, six, and twenty-four. According to their results, the incidence of moderate to severe postoperative pain was lower than that reported in our study at all-time points. The possible reason for this variation is the use of pethidine and morphine in addition to the intramuscular diclofenac and tramadol used for postoperative pain management, as reported in their study. Another possible reason may be that spinal anesthesia was not worn off since pain was assessed immediately after surgery (time zero). This finding shows that the incidence of postoperative pain could be reduced. In this study, the most commonly used analgesics were diclofenac and tramadol for postoperative pain management. This might indicate that multimodal analgesia was not used enough to treat postoperative pain in this study. Our study revealed that parturients who had abdominal field blocks were 0.035 times less likely to develop moderate to severe pain than mothers who had not received field blocks (AOR: 0.035, 95% CI: 0.009, 0.139).
In the United States of America, retrospective research revealed that 53% of patients experienced moderate to severe postoperative pain within 48 hours following cesarean delivery. According to their findings, there was a lower incidence of moderate to severe postoperative pain after a cesarean section. A possible explanation for this discrepancy is that the above study was conducted on parturients who received neuraxial anesthesia with morphine neuraxial, which resulted in a decrease in the incidence of postoperative pain compared with our results.
We found a significant relationship between preoperative anxiety and moderate to severe postoperative pain after cesarean section. This finding indicated that parturients who experienced preoperative anxiety were 2.8 times more likely to develop moderate to severe postoperative pain after cesarean section than parturients who did not experience preoperative anxiety. This finding is in line with a study from northwest Ethiopia that reported that preoperative anxiety increased the risk of moderate to severe postoperative pain in pregnant women by 2.3 times compared with that in pregnant women who were not anxious. Additionally, a Brazilian study revealed that parturients with preoperative anxiety were 1.6 times more likely to experience moderate to severe postoperative pain following a cesarean section than those without this diagnosis were. In retrospective research conducted in the United States of America, parturients who experienced preoperative anxiety were 1.93 times more likely to develop moderate to severe postoperative pain than those who did not experience it.
In this study, there was a significant association between transverse incisions and moderate to severe postoperative pain after cesarean section. This finding revealed that parturients who had transverse skin incisions were 6.9 times more likely than those who had vertical incisions to experience moderate to severe postoperative pain (AOR: 6.965, 95% CI: 2.469, 19.652). A study conducted in northwest Ethiopia revealed that Pfannenstiel incisions were more likely than midline incisions to lead to moderate to severe pain following cesarean section (AOR: 3.2, 95% CI: 1.3, 8.0). These findings are in line with our study findings. However, a prospective, double-blind, randomized, controlled study conducted in Thailand revealed that at 6 and 12 hours following surgery, the VAS score of the Pfannenstiel group was greater than that of the vertical group for repeated cesarean deliveries. Finally, they reported that the degree of postoperative pain following elective cesarean delivery was comparable whether the incision was vertical or Pfannenstiel. The difference in these results may be due to the study design, which was an RCT that compared transverse and vertical incisions among elective cesarean sections.
In this study, there was a significant relationship between a history of previous cesarean scars and moderate to severe postoperative pain following a cesarean section. This finding revealed that parturients who had a history of previous C/S scars were 3.571 times more likely to develop moderate to severe postoperative pain than those who had no history of scars (AOR: 3.571, 95% CI: 1.536, 8.300). The study supports our findings, which reported that parturients who had previously experienced CS were 2.3 times more likely to have moderate to severe pain (AOR: 2.3, 95% CI: 1.1–5). Additionally, another study revealed that parturients who underwent repeat cesarean delivery were 1.54 times more likely to experience postoperative pain than those who underwent primary cesarean delivery (1.54, 1.18 to 2.02). This may be related to more extensive surgery in the presence of scar tissue from repeat cesarean deliveries, resulting in a decreased pain threshold and increased pain sensitivity.
Conclusion
The incidence of moderate to severe postoperative pain after cesarean section was 71.2% within the first 24 hours. Parturients who had preoperative anxiety, a history of previous CS, transverse incisions, and those who did not receive an abdominal field block had moderate to severe postoperative pain after cesarean section. Preoperative anxiety should be assessed during the preoperative assessment, and appropriate interventions should be provided. Clinicians should pay special attention to parturients who have preoperative anxiety and a history of previous CS and transverse incisions. Abdominal field blocks should be provided to minimize the incidence of postoperative pain after cesarean section. Postoperative pain should be assessed, and interventions should be given on the basis of the severity of pain according to pain scale assessment.
Strengths and Limitations of the Study
The strength of this study was that it was a multicenter prospective study, so the causeâ??effect relationship was identified as a prospective study. We can generalize the results of this study to the source population since we used probability sampling. The limitation of this study was that it was not a comparative study, and parturients who underwent cesarean sections under general anesthesia were not included.
Conflict of Interest
There are no conflicts of interest.
Ethical Approval
Support letters and ethical clearance (Reference number: duirb/ 050/2023) were received from the Institutional Review Board (IRB) of Dilla University College of Medicine and Health Science before the start of the study. The importance of the study was explained, and written informed consent was obtained from each participant. Confidentiality was maintained during the study by avoiding identifiers and using codes to identify patients. The participants' involvement in the study was voluntary.
Consent for Publication
Not applicable.
Availability of Data and Material
The data used and materials to support the findings of this study are available from the corresponding author upon request.
Funding
There was no financial support from any institution to conduct this study.
Author Contribution
All the authors have made substantial contributions to the conception, design, analysis and interpretation of the study; critical review; and editing of the manuscript drafts for scientific quality and depth. All the authors have read and approved the final version of the manuscript.
Competing Interests
The authors declare that they have no competing interests.
Acknowledgments
The authors are thankful to Dilla University, The College of Health Sciences and Medicine, and the Department of Anesthesiology for all the support necessary for this work. The authors also thank all the hospitals in which the study was carried out and all the data collectors for assisting in data collection.
References
- Cunningham F, Leveno K, Bloom S, Spong CY, Dashe J. Williams obstetrics. 2014.
- Molina G, Weiser TG, Lipsitz SR, Esquivel MM, Uribe-Leitz T, Azad T, et al. Relationship between cesarean delivery rate and maternal and neonatal mortality. JAMA. 2015;314:2263-2270.
[Crossref] [Google Scholar] [PubMed]
- Gutema H, Shimye A. Cesarean section and associated factors at Mizan Aman General Hospital, Southwest Ethiopia. J Gynecol Obstet. 2014;2:37-41.
- Halil H, Abdo R, Hellil S, Kedir R. Predictors of cesarean section among women delivered at Durame General Hospital, Southern Ethiopia. J Women's Health Care. 2020;9:2167-0420.
- Merskey HE. Classification of chronic pain: Descriptions of chronic pain syndromes and definitions of pain terms. Pain. 1986.
- Villar J, Valladares E, Wojdyla D, Zavaleta N, Carroli G, Velazco A, et al. Cesarean delivery rates and pregnancy outcomes: The 2005 WHO global survey on maternal and perinatal health in Latin America. The Lancet. 2006;367:1819-1829.
- Carr DB, Goudas LC. Acute pain. The Lancet. 1999;353(9169):2051-2058.
[Crossref] [Google Scholar] [PubMed]
- Komatsu R, Carvalho B, Flood P. Prediction of outliers in pain, analgesia requirement, and recovery of function after childbirth: A prospective observational cohort study. Br J Anaesth. 2018;121(2):417-426.
[Crossref] [Google Scholar] [PubMed]
- Bateman BT, Franklin JM, Bykov K, Avorn J, Shrank WH, Brennan TA, et al. Persistent opioid use following cesarean delivery: Patterns and predictors among opioid-naïve women. Am J Obstet Gynecol. 2016;215(3):353.e1–353.e18.
[Crossref] [Google Scholar] [PubMed]
Citation: Moreda D, Sagni Y, Amsalu H, Molla S (2025) Incidence and Predictors of Moderate to Severe Postoperative Pain after Cesarean Section among Parturient Receiving Spinal Anesthesia at the Selected Southern Ethiopian Governmental Hospital 2023: A Multicenter Prospective Single-Armed Cohort Study. J Pain Manage Med. 12:366.
Copyright: © 2025 Moreda D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.